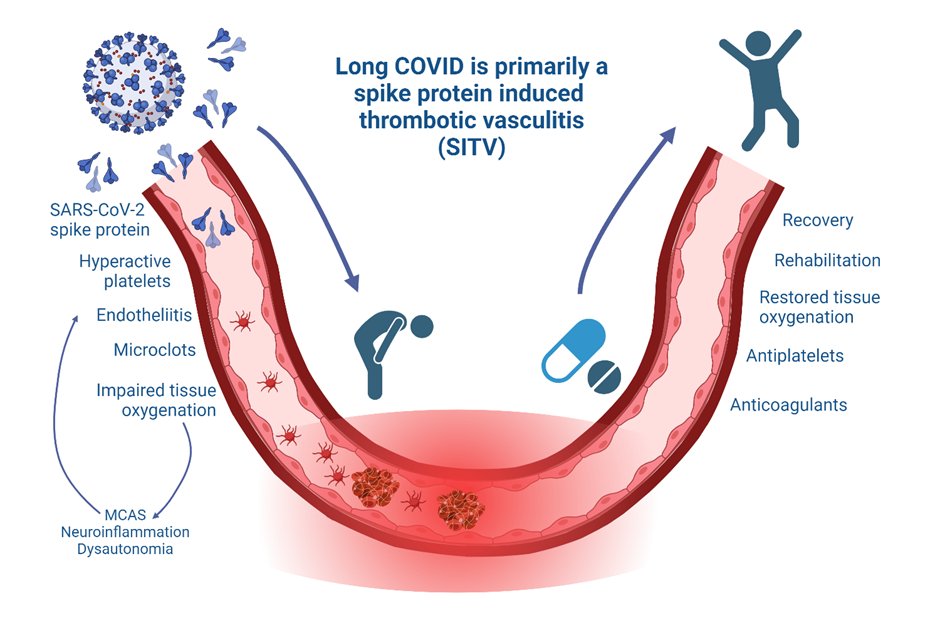
Long covid is primarily a spike protein-induced thrombotic vasculitis, & we use Robin as a supporting case study.
We start by discussing the highly thrombotic nature of acute COVID & how this pathology doesnt cease in those with long COVID. in other words, long COVID is a continuation of the pathology accompanying acute COVID. Importantly, we cant rehabilitate until the pathology is treated we highlight the role of microclots in capillary occlusion, that coagulopathic outcomes occur after acute covid (e.g. ↑ stroke risk), that there is platelet hyperactivation and endotheliitis, and all this leads to impaired oxygen extraction (and more) to complicate things, we briefly discuss other core co-pathologies: dysautonomia and POTS, and MCAS. We discuss that coagulopathy can be implicated in these diseases, for example, tryptase has a role in fibrinolysis.
Since similar pathologies occur with the covid vaccines, we propose spike protein may have a unique role in aetiology of long COVID Based on limited evidence, those with LongCovid & postvac seem to be unable to clear spike protein (/whole virion). We feel this offers clues…
We therefore propose the use of the term “Spike protein-induced Thrombotic Vasculitis” or “SITV” Naming things gets very heated, but this has some benefits:
1. It clearly describes the pathology
2. Provides focus for targeted treatment
3. Offers a distinction for subtypes of LC
This 3rd point is important. Whilst we do believe that long COVID is predominated by coagulopathy, we fully acknowledge this may not be the primary pathology for EVERYONE. lots of work is characterising subtypes, we feel characterising by primary pathology can be useful
We then discuss treatment targets: Anticoagulants, particularly heparin due to its affinity to spike protein, and dabigatran due to its enhanced fibrinolytic properties Antiplatelets, particularly P2Y12 inhibitors (e.g. clopidogrel) and aspirin.
We also note aspirin has previously been investigated to reduce vaccine-induced (acute) endotheliitis Antidepressants (SSRIs), particularly sertraline. SSRIs reduce endothelial inflammatory markers (e.g. IL-8), binds to S1 subunit of the spike protein, have antiplatelet effects, mast cell stabilising effects, and anti-neuroinflammatory effects. the antiplatelet and endothelial effects seem enhanced in combination with aspirin or clopidogrel so to be clear, we are interested in SSRIs because of their role in coagulopathic mechanisms!
In line with others, we believe early and aggressive treatment is needed. At the lack of RCTs, we present Robin’s case. After > 20 months of hell, he started aggressive triple therapy. he initially declined as many do, but then recovered
Then he got his second infection. All hell broke loose again. a less aggressive treatment regime did not help him, but triple therapy + SSRIs (as a third antiplatelet) did. He returned to work and exercise.
Then got infection number 3 and recovered rapidly with aggressive antiplatelet treatment
Whilst we don’t think coagulopathy is the ONLY thing going wrong in EVERYONE with long COVID, we think this is a primary problem in many patients, and should be treated aggressively and early if possible This does not preclude fully exploring and treating other co-pathologies…
Our perspective does give examples of how coagulopathy can interact with other co-pathologies, creating a vicious cycle between lots of factors. there are many other things going on as well as other treatments worthy of exploration too, which we didn’t discuss in detail
We hope this is an interesting and useful paper. We will be submitting to journals soon, so we welcome feedback (bearing in mind we have word limits and can’t discuss it all!). (Robin’s email is on the manuscript)
To be clear: theres lots of treatment targets. The ones we discuss are (mostly) the ones useful for Robins case as publishing that was the initial point of the paper, & then we decided to turn that into a perspective piece. Patients should be treated for their indiv needs ofc!
Treatment aimed at fixing the problem(s): inflammation, coagulopathy, and mitochondrial energy issues: Treat the spike (antiviral/natto). Treat the coag/microclots (natto,asa, plavix).Treat the M1 immune shift inflammation: metformin, melatonin, arb, fisetin