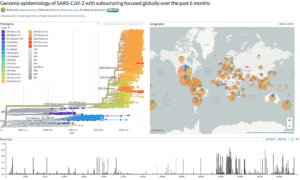
COVID-19 has reached a “pseudo-endemic” state. Is the C-19 emergency over?
You cannot end a pandemic of this virus without achieving herd immunity.
After a natural pandemic, the population eventually reaches endemicity, a state where the virus can no longer spread widely due to herd immunity.
With the influenza virus, this transition occurs, and it typically only returns in seasonal outbreaks. However, these outbreaks are immediately controlled because of the established herd immunity in the population. Influenza does not reemerge with increased virulence or cause more severe disease because it is quickly controlled by the population’s herd immunity. Only a small section of the population, who no longer have those antibodies, generally get infected and have to recall them.
Each year, multiple strains of the influenza virus circulate globally. These strains are primarily categorized into two types: influenza A and influenza B.
- New Flu Strains: Typically, the World Health Organization (WHO) identifies and monitors two to four new influenza strains each year to be included in the seasonal flu vaccine. These strains are chosen based on global surveillance and predictions of which strains are most likely to circulate in the upcoming flu season.
- Old Flu Strains: Many older strains of influenza continue to circulate alongside newer ones. Influenza viruses undergo continuous genetic changes through a process called antigenic drift, resulting in minor changes to the virus over time. This means that while certain strains may dominate in a given year, variants of older strains often remain in circulation.
In contrast, the endemic stage of COVID-19 presents a unique challenge. While the current strains are less severe, the virus continues to evolve, posing the risk of new pathways to severe disease emerging at any time. This situation is unprecedented because the COVID-19 virus is still evolving, and the so-called endemic state is misleading. Unlike endemic influenza, which is subject to seasonal triggers and controlled by herd immunity, COVID-19 has reached a “pseudo-endemic” state and is not controlled by herd immunity. The spread is a little less, the virulence has been less since Omicron but it is spreading in enough volume in the population to say that we have not reached herd immunity. It is not limited by seasonal patterns and has the potential to trigger severe disease in the vaccinated population at any time.
Endemic Influenza
- Seasonality: Influenza is typically seasonal, with peaks in colder months (winter) in temperate regions. This predictability helps in planning and managing healthcare resources.
- Predictability: The virus’s impact is somewhat predictable year-to-year in terms of when and where outbreaks will occur.
- Severity: While influenza can cause severe disease, particularly in vulnerable populations (e.g., elderly, young children, immunocompromised individuals), it generally follows a well-understood pattern.
- Vaccination and Immunity: Seasonal vaccines are updated annually to match circulating strains, and population immunity plays a significant role in controlling outbreaks.
Pseudo-Endemic COVID-19
- Lack of Seasonality: COVID-19 does not follow a strict seasonal pattern. Outbreaks can occur at any time, influenced by various factors such as new variants, public health measures, and population behavior.
- Unpredictability: The virus can cause sudden and severe outbreaks, making it harder to predict and manage.
- Severity: COVID-19 has shown the capacity to cause severe disease across all age groups, although with varying degrees of risk. Long COVID and severe acute respiratory syndrome are notable risks that can arise unpredictably.
- Variants: The emergence of new variants with different transmissibility and immune evasion properties adds a layer of unpredictability. These variants can lead to sudden spikes in cases and hospitalizations.
- Vaccination and Immunity: Most people in Western countries were vaccinated. While the vaccines may have been effective initially, they did not generate herd immunity. Breakthrough infections became more frequent, and the virus continues to mutate (not under control). It is only a matter of time before more severe disease breaks out.
Key Differences
- Seasonality vs. Non-Seasonality: Influenza has a clear seasonal pattern; COVID-19 does not.
- Predictability: Influenza outbreaks are more predictable; COVID-19 outbreaks can be sudden and severe at any time.
- Triggers for Severe Disease: Severe influenza is often linked to seasonal outbreaks, whereas COVID-19 can cause severe disease spikes due to new variants or changes in public health measures.
- Management and Preparedness: Influenza management relies on seasonal preparedness; COVID-19 requires continuous vigilance and adaptability due to the mistake of a mass vaccination campaign with suboptimal vaccines (none neutralising).
Understanding these differences is crucial for public health strategies and preparedness, as the approach to managing an endemic influenza differs significantly from managing the ongoing challenges posed by COVID-19.